Services
DIAGNOSTIC SERVICES

- 1Visual acuity check (Snellen, EDTRS)
Alternative Names : Eye test – acuity; Vision test – acuity; Snellen test

The visual acuity test is used to determine the smallest letters you can read on a standardized chart (Snellen chart) or a card held 20 feet (6 meters) away.
Special charts are used when testing at distances shorter than 20 feet (6 meters). Some Snellen charts are actually video monitors showing letters or images.
The visual acuity test is a routine part of an eye examination or general physical examination, particularly if there is a change in vision or a problem with vision.
 In children, the test is performed to screen for vision problems. Vision problems in young children can often be corrected or improved. Undetected or untreated problems may lead to permanent vision damage.
In children, the test is performed to screen for vision problems. Vision problems in young children can often be corrected or improved. Undetected or untreated problems may lead to permanent vision damage.There are other ways to check vision in very young children, or in people who do not know their letters or numbers.
A Snellen chart is an eye chart that can be used to measure visual acuity. Snellen charts are named after the Dutch ophthalmologist Herman Snellen who developed the chart in 1862. Many ophthalmologists and vision scientists now use an improved chart known as the LogMAR chart.
ETDRS stands for Early Treatment Diabetic Retinopathy Study. The ETDRS test is designed to eliminate inaccuracies in the Snellen and Sloan tests.
Normal Results
Visual acuity is expressed as a fraction.
- The top number refers to the distance you stand from the chart. This is often 20 feet (6 meters).
- The bottom number indicates the distance at which a person with normal eyesight could read the same line you correctly read.
For example, 20/20 is considered normal. 20/40 indicates that the line you correctly read at 20 feet (6 meters) away can be read by a person with normal vision from 40 feet (12 meters) away. Outside of the United States, the visual acuity is expressed as a decimal number. For example, 20/20 is 1.0, 20/40 is 0.5, 20/80 is 0.25, 20/100 is 0.2, and so on.
Even if you miss one or two letters on the smallest line you can read, you are still considered to have vision equal to that line.
What Abnormal Results Mean
Abnormal results may be a sign that you need glasses or contacts. Or it may mean that you have an eye condition that needs further evaluation by a provider.
- 2Refraction (prescription of glasses for distant and near vision)
Refraction is an eye exam that measures a person’s prescription for eyeglasses or contact lenses.
How the Test is performed
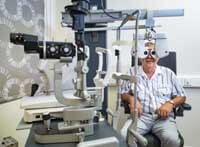 An ophthalmologist or optometrist performs this test. Both of these professionals are often called “eye doctor.”
An ophthalmologist or optometrist performs this test. Both of these professionals are often called “eye doctor.”You sit in a chair that has a special device (called a phoroptor or refractor) attached to it. You look through the device and focus on an eye chart 20 feet (6 meters) away. The device contains lenses of different strengths that can be 4moved into your view. The test is performed one eye at a time.
The eye doctor will then ask if the chart appears more or less clear when different lenses are in place.
- 3Tonometry (measurement of intraocular pressure)
Alternative Names: Intraocular pressure (IOP) measurement; Glaucoma test; Goldmann applanation tonometry (GAT)
Tonometry measures the pressure within your eye. During tonometry, eye drops are used to numb the eye. Then a doctor or technician uses a device called a tonometer to measure the inner pressure of the eye. A small amount of pressure is applied to the eye by a tiny device or by a warm puff of air.
The range for normal pressure is 12-22 mm Hg (“mm Hg” refers to millimeters of mercury, a scale used to record eye pressure). Most glaucoma cases are diagnosed with pressure exceeding 20mm Hg. However, some people can have glaucoma at pressures between 12 -22mm Hg. Eye pressure is unique to each person.
- 4Slit lamp examination
Alternative Names: Biomicroscopy
The slit-lamp examination looks at structures that are at the front of the eye.
The slit-lamp is a low-power microscope combined with a high-intensity light source that can be focused as a thin beam.
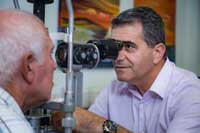 You will sit in a chair with the instrument placed in front of you. You will be asked to rest your chin and forehead on a support to keep your head steady.
You will sit in a chair with the instrument placed in front of you. You will be asked to rest your chin and forehead on a support to keep your head steady.The eye doctor will examine your eyes, especially the eyelids, cornea, conjunctiva, sclera, and iris. Often a yellow dye (fluorescein) is used to help examine the cornea and tear layer. The dye is either added as an eye drop. Or the provider may touch a fine strip of paper stained with the dye to the white of your eye. The dye rinses out of the eye with tears as you blink.
Next, drops may be placed in your eyes to widen (dilate) your pupils. The drops take about 15 to 20 minutes to work. The slit-lamp examination is then repeated using another small lens held close to the eye, so the back of the eye can be examined.
- 5Ophthalmoscopy
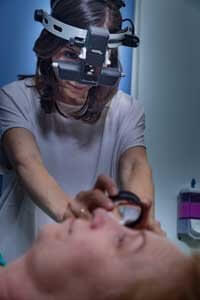 Ophthalmoscopy is an examination of the back part of the eye (fundus), which includes the retina, optic disc, choroid, and blood vessels.
Ophthalmoscopy is an examination of the back part of the eye (fundus), which includes the retina, optic disc, choroid, and blood vessels.There are different types of ophthalmoscopy.
- Direct ophthalmoscopy. You will be seated in a darkened room. The health care provider performs this exam by shining a beam of light through the pupil using an instrument called an ophthalmoscope. An ophthalmoscope is about the size of a flashlight. It has light and different tiny lenses that allow the provider to view the back of the eyeball.
- Indirect ophthalmoscopy. You will either lie or sit in a semi-reclined position. The provider holds your eye open while shining a very bright light into the eye using an instrument worn on the head. (The instrument looks like a miner’s light.) The provider views the back of the eye through a lens held close to your eye. Some pressure may be applied to the eye using a small, blunt probe. You will be asked to look in various directions.
- 6Contact Lenses fitting for refractive errors and Keratoconus
Contact lenses are thin, clear disks of plastic that float on the surface of the eye. They correct vision like eyeglasses do and are safe when used with care. Contact lenses are used to correct the same conditions that eyeglasses do: myopia (nearsightedness), hyperopia (farsightedness), astigmatism (blurred vision due to the shape of the cornea) and presbyopia (inability to see close up). There are also certain eye conditions, such as keratoconus (when the cornea develops a cone-like bulge) and aniseikonia (when each eye perceives the size of an image differently) that are better corrected with contact lenses.
Millions of people around the world wear contact lenses. Depending on your lifestyle, your motivation and the health of your eyes, contact lenses may provide a safe and effective alternative to eyeglasses when used with proper care and maintenance.
- 7Orthokeratology
Alternative names: Orhto-K, Overnight Vision Correction, Corneal Refractive Therapy and CRT.
Orthokeratology: is a non-surgical procedure using specially designed contact lenses to gently reshape the curvature of the eye to improve vision.
This is a revolutionary non-surgical procedure that eliminates the need for glasses or daytime contact lenses. It improves vision by gently reshaping your eye WHILE YOU SLEEP using specially designed therapeutic contact lenses. You just put the specially fitted lenses in at bedtime, and when you awake, you will have clear, sharp, natural vision for your waking hours. This safe and effective treatment can correct near-sightedness (including high prescriptions), farsightedness, astigmatism and presbyopia (blurred near vision). It is a great alternative to LASIK for those who don’t want the risk or are not ready for surgery.
- 8Orthoptic assessment in adults and children
Orthoptists are eye health professionals who care for patients with eye disorders. Through a unique set of skills, orthoptists play a crucial role in the detection, diagnosis and management of eye diseases in both adults and children. An orthoptic eye exam is done to measure how much the eye turns from various positions. Orthoptist tests are diagnostic tests performed to assess certain conditions like squint, lazy eye, double vision, eye movement disorders, cataract, glaucoma, refractive errors, vision disabilities due to neurological disorders and diabetic eye diseases. The tests assess vision, eye alignment, eye movement and binocular vision.
 An orthoptic exam provides information to your ophthalmologist on:
An orthoptic exam provides information to your ophthalmologist on:- Amblyopia (lazy eye)
- Binocular vision (not being able to use your eyes together)
- Abnormal eye moments (caused by injury or disease)
- Diplopia (double vision)
- 9Retinoscopy
Alternative name: skiascopy
Is a technique to objectively determine the refractive error of the eye (farsighted, nearsighted, astigmatism) and the need for glasses. The test can be quick, easy, and reliably accurate and requires minimal cooperation from the patient.
How is it performed?
A hand held instrument called a retinoscope projects a beam of light into the eye. When the light is moved vertically and horizontally across the eye, the examiner observes the movement of the reflected light from the back of the eye. This reflection is called red reflex. The examiner then introduces lenses in front of the eye and as the power of the lenses changes, there is a corresponding change in the direction and pattern of the reflection. The examiner keeps changing the lenses until reaching a lens power that indicates the refractive error of the patient.
When is retinoscopy used?
Retinoscopy is used to determine refractive error in children, developmentally delayed adults, or in individuals whose behavior limits the ability to be cooperative with autorefraction or subjective refraction. It is especially useful in very young children and infants.
- 10Contrast sensitivity test
Contrast sensitivity is a very important measure of visual function, especially in situations of low light, fog or glare, when the contrast between objects and their background often is reduced. Driving at night is an example of an activity that requires good contrast sensitivity for safety.
A contrast sensitivity test measures your ability to distinguish between finer and finer increments of light versus dark (contrast).
This differs from common visual acuity testing in a routine eye exam, which measures your ability to recognize smaller and smaller letters on a standard eye chart. Contrast sensitivity is a very important measure of visual function, especially in situations of low light, fog or glare, when the contrast between objects and their background often is reduced. Driving at night is an example of an activity that requires good contrast sensitivity for safety.
Even if you have 20/20 visual acuity, you can have eye or health conditions that may diminish your contrast sensitivity and make you feel that you are not seeing well.
Contrast sensitivity testing often isn’t included in a routine eye exam. Your eye doctor might perform the test because of a specific visual complaint you have or because he or she suspects you have a condition that is affecting your ability to discern contrast
- 11Endotheliometry (Topcon)
Alternative names: spectral microsocopy
Specular microscopy is a noninvasive photographic technique that allows you to visualize and analyze the corneal endothelium. Using computer-assisted morphometry, modern specular microscopes analyze the size, shape and population of the endothelial cells.
The corneal endothelium is a single cell layer on the innermost surface of the cornea. A given number or density of endothelial cells is present at birth, usually about 5,000 cells per square millimeter. There is a normal, progressive and slow loss of endothelial cells with aging.
- 12Pachymetry
Alternative names: central corneal thickness-CCT
Corneal pachymetry is the process of measuring the thickness of the cornea. A pachymeter is a medical device used to measure the thickness of the eye’s cornea.
It is used to perform corneal pachymetry prior to refractive surgery (for ensuring sufficient corneal thickness to prevent abnormal bulging of the cornea, a side effect known as ectasia), for Keratoconus screening, LRI surgery (Limbal Relaxing Incisions – is used to reduce corneal astigmatism by placing a pair of incisions of a particular depth and arc length at a steep axis of corneal astigmatism) and is useful in screening for patients suspected of developing glaucoma among other uses.
- 13Biometry –IOL master
This is a test to measure the shape and size of the eye. It is commonly used to calculate the power of intraocular lens (IOL) implants required for cataract and refractive surgery. Biometry can be performed using either optical coherence interferometry or ultrasound technology.
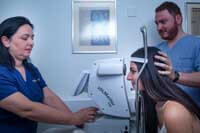 At our clinic we use the state of the art Zeiss IOL Master 700 (optical coherence interferometry). This equipment is able to measure the length of the eyeball (axial length), curvature of the cornea (keratometry), anterior chamber depth and white to white (corneal width). It uses several different formulas to give the surgeon options as to IOL lens powers for each individual eye.
At our clinic we use the state of the art Zeiss IOL Master 700 (optical coherence interferometry). This equipment is able to measure the length of the eyeball (axial length), curvature of the cornea (keratometry), anterior chamber depth and white to white (corneal width). It uses several different formulas to give the surgeon options as to IOL lens powers for each individual eye. - 14Ultrasound (A-scan, B-scan)
Alternative Names: Echography – eye orbit; Ultrasound – eye orbit; Ocular ultrasonography; Orbital ultrasonography
An eye and orbit ultrasound uses high-frequency sound waves to measure and produce detailed images of your eye.
An A-scan ultrasound measures the eye to determine the right power of a lens implant before cataract surgery.
A B-scan is done to look at the inside part of the eye or the space behind the eye that cannot be seen directly. This may occur when you have cataracts or other conditions that make it hard for the doctor to see into the back of your eye. The test may help diagnose retinal detachment, tumors, or other disorders.
- 15Ultrasound Biomicroscopy – UBM (Aviso)
 Ultrasound biomicroscopy (UBM) is an excellent tool for imaging the more anterior portion of the posterior segment of the eye, namely, the ciliary body, lens and posterior iris. These areas are difficult, if not impossible, to see with traditional imaging devices.
Ultrasound biomicroscopy (UBM) is an excellent tool for imaging the more anterior portion of the posterior segment of the eye, namely, the ciliary body, lens and posterior iris. These areas are difficult, if not impossible, to see with traditional imaging devices. - 16Corneal topography and tomography (Allegro topolyzer)
Alternative names: photokeratoscopy or videokeratography
 It is a non-invasive medical imaging technique for mapping the surface curvature of the cornea, the outer structure of the eye. Since the cornea is normally responsible for some 70% of the eye’s refractive power, its topography is of critical importance in determining the quality of vision and corneal health.
It is a non-invasive medical imaging technique for mapping the surface curvature of the cornea, the outer structure of the eye. Since the cornea is normally responsible for some 70% of the eye’s refractive power, its topography is of critical importance in determining the quality of vision and corneal health.Oculus Pentacam Scan: The Pentacam is a comprehensive eye scanner which provides data critical to the planning of the treatment.
The Pentacam images the anterior segment of the eye by a rotating Scheimpflug camera measurement. This rotating process supplies pictures in three dimensions. The center of the cornea is measured very precisely because of this rotational imaging process. The measurement process lasts less than two seconds, and minute eye movements are captured and corrected simultaneously. By measuring 25,000 true elevation points, precise representation, repeatability and analysis are guaranteed.
The Pentacam provides 3-dimensional chamber analysis of the complete anterior segment of the eye, corneal topography of both the front and the back of the cornea, thickness measurements across the entire diameter of cornea. It also can provide cataract analysis and clearly detect corneal disorders such as Keratoconus, where laser vision correction is sometimes not appropriate.
- 17Eye wavefront analysis (Zywave analyzer)
Alternative names: aberrometry
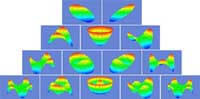 Wavefront mapping is the technology that makes custom laser eye surgery possible by precisely measuring and diagraming the imperfections of an optical system, such as the eye. These imperfections are divided into lower-order aberrations, such as myopia, hyperopia, and astigmatism, and higher-order aberrations that affect night vision.
Wavefront mapping is the technology that makes custom laser eye surgery possible by precisely measuring and diagraming the imperfections of an optical system, such as the eye. These imperfections are divided into lower-order aberrations, such as myopia, hyperopia, and astigmatism, and higher-order aberrations that affect night vision.Wavefront analyzers are used to map aberrations in the eye. Several types of visual imperfections, referred to as lower and higher-order aberrations, exist within the eye and can affect both visual acuity and the quality of vision. Prior to wavefront technology, only lower-order aberrations such as myopia, hyperopia, and astigmatism could be measured and treated. However, these do not account for all potential vision imperfections. Higher-order aberrations can also have a significant impact on quality of vision and are often linked to glare and halos that may cause night vision problems. Wavefront analyzers use a Hartmann-Shack sensor, which maps both lower and higher-order aberrations by projecting waves of light into a patient’s eye and mapping the waves that bounce back through the pupil. A perfect wavefront would be completely flat. When light rays enter the eye and traverse the different refractive indices, the wavefront surface changes, taking on a shape unique to that eye. These variations are called wavefront aberrations.
- 18Visual fields (Humphrey Field Analyzer)
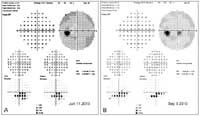 A visual field test is a method of measuring an individual’s entire scope of vision, that is their central and peripheral (side) vision. Visual field testing maps the visual fields of each eye individually and can detect blind spots (scotomas) as well as more subtle areas of dim vision. The visual field test is a subjective examination, so the patient must be able to understand the testing instructions, fully cooperate, and complete the entire test in order to provide useful information.
A visual field test is a method of measuring an individual’s entire scope of vision, that is their central and peripheral (side) vision. Visual field testing maps the visual fields of each eye individually and can detect blind spots (scotomas) as well as more subtle areas of dim vision. The visual field test is a subjective examination, so the patient must be able to understand the testing instructions, fully cooperate, and complete the entire test in order to provide useful information.Visual field testing is most frequently used to detect signs of glaucoma damage to the optic nerve. In addition, visual field tests are useful for detection of central or peripheral retinal diseases of the retina, eyelid conditions such as drooping (ptosis), optic nerve damage and disease, and conditions affecting the visual pathways from the optic nerve to the area of the brain (occipital cortex) where this information is processed into vision
- 19OCT disc and macula (Cirrus-Zeiss)
Optical coherence tomography (OCT) is a non-invasive imaging test. OCT uses light waves to take cross-section pictures of your retina.
With OCT, your ophthalmologist can see each of the retina’s distinctive layers. This allows your ophthalmologist to map and measure their thickness. These measurements help with diagnosis. They also provide treatment guidance for glaucoma and diseases of the retina. These retinal diseases include age-related macular degeneration (AMD) and diabetic eye disease.
- 20OCTA-OCT Angiography (Spectralis HRA+OCT imaging platform-Heidelberg Engineering)
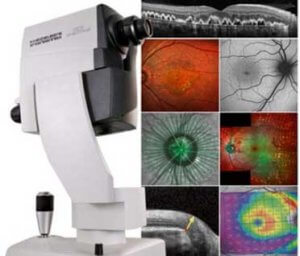 The SPECTRALIS is an expandable diagnostic imaging platform which combines laser fundus imaging with high resolution OCT.
The SPECTRALIS is an expandable diagnostic imaging platform which combines laser fundus imaging with high resolution OCT.Options include: anterior segment OCT (corneal layers, angle structures)
glaucoma module (optic nerve head, RNFL, ganglion cell layer, compares to a reference database of normal eyes)
OCT2 module for the retina (high scan rate 85000 Hz provides excellent image quality and significantly improved acquisition speed)
Fundus (multicolor imaging, infrared imaging)
Angiography (widefield imaging, fluorescein angiography, ICG angiography)
OCT-angiography (OCT-A: a new diagnostic tool and heavily promoted as an alternative or an adjunct to classic fluorescein angiography (FA). It is a fast imaging tool, detecting streaming blood, thereby allowing to construct an image of the retinal vasculature; in contrast to “classical” FA it is dye-free, and therefore lacks significant side effects associated with the fluorescein injections such as such as vomiting, hypersensitivity reactions and cardiovascular complications. This new technology allows the in situ, high-resolution visualization of the individual vascular layers. In contrast to FA, which displays only the superficial capillary network, OCT-A visualizes the superficial, the deep and the choroidal vascular network; even the middle capillary plexus can be identified)
- 21Wide field fluorescein angiography (Spectralis HRA, Heidelberg Engineering)
SPECTRALIS scanning laser angiography can be conducted with either fluorescein or ICG dye. Both modes produce detailed, high resolution images and video sequences that show vessel filing, flow and leakage.
The widefield Imaging Module provides a 55-degree field of view for all fundus imaging capturing the macula, the optic nerve head and areas beyond the vessel arcades in a single image. The high-resolution, high-contrast scanning laser images captured with this SPECTRALIS module offer diagnostic capabilities beyond those of conventional fundus photography
- 22Electrodiagnostics – EDTs (ERG, EOG, VEP)
Electrodiagnosis is a method of obtaining information about diseases by recording the electrical activity of eye in response to visual stimulation. The electrical activity is recorded painlessly by attaching sticky electrodes to the skin around the eye. The information is used to accurately diagnose a number of eye conditions and monitor their progress.
Visual Evoked Potential (VEP)
This is a test of the pathway between the eye and the vision area at the back of the brain. We will record the electrical signals produced naturally by your brain when looking at a visual stimulus (patterns or lights).
ElectroRetinoGram (ERG)
This is a test of the retina (the light sensitive layer) at the back of the eye. We record the electrical signals produced naturally by the retina in response to a flash of light.
ElectroOculoGram (EOG)
This is also a test of the retina of the eye, but we record the electrical signals produced by the eye when you move your eye from side to side.
PROCEDURES OFFERED
- 1Femtosecond laser assisted cataract surgery –FLACS (LenSx-ALCON)
- 2Phacoemulsification (Centurion Vision System – ALCON)
- 3Vitrectomy
Vitrectomy is a procedure performed to remove the vitreous jelly from the eye. Most commonly this is performed to treat pathological conditions of the retina such as macular hole and epi retinal membrane, retinal detachment, diabetic retinopathy and others. The vitreous jelly removed is replaced either with fluid, gas or silicone oil depending on the pathology present.
- 4Retinal detachment repair
The retina is the inner most layer of the back of the eye. It consists of layers of nerve cells and blood vessels and it is the seeing part of the eye. Light is focused on the retina, the retina forms an image which it sends to the brain via the optic nerve. The retina can detach become torn and detach from the wall of the eye and this needs to be surgically repaired otherwise it will lead to blindness. There are various methods of retinal detachment repair which may or may not involve a vitrectomy.
- 5Anti-VEGF injections –AVASTIN, LUCENTIS, EYLEA
- 6Femtosecond LASIK (visumax-ZEISS)
- 7Cornea Refractive Surgery –PRK, LASIK (Alegretto WAVELIGHT)
- 8Conreal Cross Linking for keratoconus (PESCHKE-Platinum PXL)
- 9Pterygium and limball transplantation surgery
Pterygium
Pterygium is a pink tissue and it typically starts on the cornea near the nose. The exact cause is unknown, but it is associated with excessive exposure to sunlight. Symptoms of pterygium include redness, foreign body sensation, tearing, dry eyes or decreased vision from irregular astigmatism.
A small atrophic pterygium may be treated with artificial tears.
Conjunctival auto-grafting is recognized by many corneal and anterior segment surgeons as the procedure of choice for pterygium surgery (auto-grafting covers the bare sclera with conjunctival tissue that is surgically removed from an area of healthy conjunctiva). An excellent cosmetic result is obtained with this technique.
- 10Corneal transplantation Full thickness transplantation (PKP) and partial thickness transplantation (DESAEK,DEAMEK)
Keratoplasty (PKP, DALK, DSAEK)
Keratoplasty (corneal transplantation):
Keratoplasty is a procedure, when a damaged cornea, is replaced by a donor graft.
Reasons to proceed with a corneal transplantation are: corneal scarring because of an injury or an infection, corneal ulcers, a medical condition that makes your cornea bulge out (keratoconus), thinning, clouding, or swelling of the cornea, inherited eye diseases, such as Fuchs’ dystrophy and others, problems caused by an earlier eye operation.
PKP (penetrating keratoplasty): the entire cornea is replaced
DALK (deep anterior lamellar keratoplasty): the anterior part of the cornea is replaced
DSAEK (descemet’s stripping automated keratoplasty): the posterior part of the cornea is replaced
- 11Amniotic Membrane Transplantation
Amniotic membrane is the inner layer of the placenta and it is a thin, avascular tissue which aids healing and inhibits inflammation and scarring.
Indications for amniotic membrane transplantations are as a graft in conjunctival reconstruction; a graft in corneal surface reconstruction; a patch in corneal surface reconstruction; as a substrate in association with limbal transplant in limbal stems cells deficiency (e.g. after an eye burn) and as a barrier in bullous keratopathy in eyes with poor potential (in combination with corneal micropuncturing).
- 12Trabeculectomy
- 13Cyclodiode laser ablation
- 14Ahmed glaucoma valve implant
- 15Lid surgery
- 16Dacryocystorhinostomy –DCR
- 17Other Oculoplastic surgeries
- 18Retinal Photocoagulation (PASCAL Laser system)
- 19YAG-Laser system (ZEISS)